 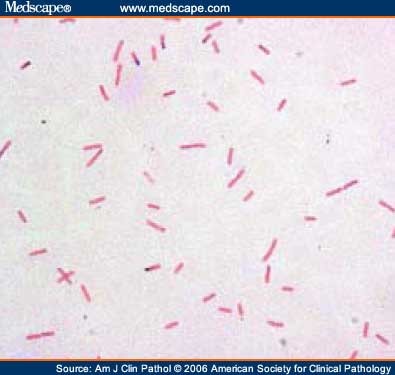 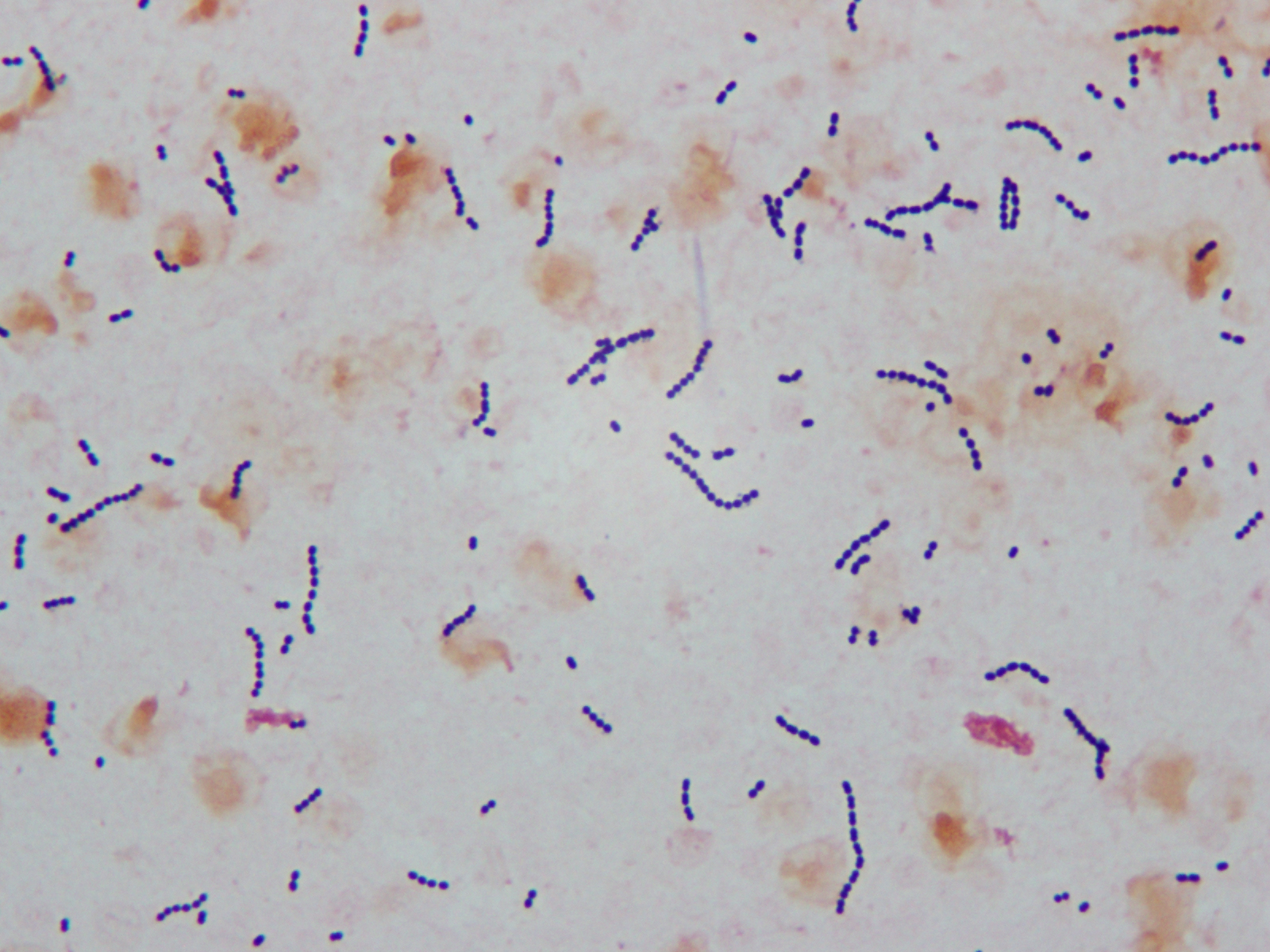
Identifying pathogens causing Boodstream Infection (BSI) in patients undergoing chemotherapy and determining the risk factors for infections by CRGN bacteria is essential to understand which patients would benefit from early initiation of antibiotics with activity against these organisms. 5 The main challenge is accurately identifying patients at high risk for these infections and the timely institution of adequate antimicrobial therapy. Therefore, physicians must judiciously and appropriately use these last-line antimicrobials. The benefit of empirically covering carbapenem-resistant GNB during FN should outweigh the risk of increasing the selective pressure for bacterial resistance. Old drugs, such as polymyxins and aminoglycosides, can be used however, they are highly toxic. However, some of these antibiotics are either unavailable, or their use is cost-prohibitive in low-income and developing countries. 6 Therapeutic options for these infections usually rely on drugs such as new beta-lactam/beta-lactamase inhibitors with activity against Class A-producing carbapenemase bacteria. The indications for empirical antibiotic coverage for Carbapenem-Resistant Gram-Negative (CRGN) bacteria in patients with FN are not well defined and should be based on local epidemiology and individual risk factors. 3, 4 Antibiotic resistance among GNB, especially carbapenem resistance due to carbapenemase production, such as Klebsiella pneumoniae Carbapenemase (KPC) or New-Delhi Metallo-beta-lactamase (NDM), is currently a major therapeutic challenge. 
2 Bacterial infections are most prevalent in this scenario, with Gram-Negative Bacteria (GNB) accounting for a high proportion of cases. 1 Infection-related mortality remains high in patients with Febrile Neutropenia (FN), accounting for up to 55% of all cases. Despite the advances, chemotherapy remains essential for cancer treatment, which may increase the number of patients with neutropenia and severe infections. In recent years, the prognosis of patients with oncological diseases has significantly improved with the development of new therapeutic options. ConclusionsĪ CRGN risk-guided approach should be considered for empirical antibiotic therapy in patients with FN. Patients with CRGN BSI received 75% less empirical active antibiotics and had 27.2% higher 30-day mortality rates than controls. Variables related to CRGN BSI in Cox regression analysis were the first chemotherapy session ( p<0.01), chemotherapy performed in the hospital setting ( p = 0.03), intensive care unit admission ( p<0.01), and CRGN isolation in the previous year ( p<0.01). From 105 patients included in the case-control analysis, all cases had baseline hematological malignancies (60% acute myeloid leukemia). Gram-negative bacteria accounted for 537 (35.5%) of the isolated bacteria, of which 93 (17.3%) were carbapenem-resistant. Resultsįrom 6094 blood cultures evaluated, 1512 (24.8%) showed positive results. Each case was matched to two controls from whom CRGN were not isolated and had the same sex and year of inclusion in the study. Predictors of CRGN were evaluated through a case-control analysis. We characterized pathogens causing BSI in patients aged ≥18 years who had undergone systemic chemotherapy for solid or hematological cancers between 20 in Porto Alegre, Brazil. Carbapenem-Resistant Gram-Negative (CRGN) Bloodstream Infections (BSI) represent a therapeutic challenge, especially in the context of Febrile Neutropenia (FN) in cancer patients. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
